Our physiatrists offer a variety of diagnostic and non-operative pain management options, including ultrasound-guided injections, regenerative medicine, therapeutic neural blockade and acupuncture. These may be prescribed in combination or alone. Our physicians also work in partnership with local physical therapists and other professionals to offer comprehensive pain management treatment.
Regenerative Medicine
Musculoskeletal degeneration and complications from injuries have become more prevalent as people live longer and increasingly participate in more rigorous athletic and recreational activities. At the Center for Spine and Orthopedics, we strive to offer our patients a wide array of non-surgical treatment options, including regenerative medicine, such as platelet-rich plasma (PRP) therapy. PRP has been around since the mid 1990’s and is the most common type of regenerative medicine as well as the most studied.
What is regenerative medicine?

Stem cells are most commonly harvested from a patient’s bone marrow or fat, both of which require a surgery center and anesthesia. The use of stem cells harvested from placental tissue involves an in-office procedure not requiring a surgery center or anesthesia. PRP involves an approximately 30-minute in-office procedure without anesthesia.
What types of regenerative medicine are offered at CSO?
Our board-certified pain management specialists offer PRP injections for hip, knee, foot and ankle, hand, and shoulder joints and the facets of the cervical (neck) and lumbar (lower back) spine. They also administer other stem cell injections, including those harvested from abiotic stem cells and stem cells harvested via bone marrow biopsy.
Why CSO for regenerative medicine?
The key to effectively administering regenerative medicine injections is the placement of the injection at the exact point of injury. Our specialists, Dr. George Leimbach and Dr. Paul Leo, each have 30 years of experience giving injections, and they have a 99 percent track record of success. To ensure that PRP gets to the exact injury site, they administer PRP very precisely, using image guidance with ultrasound or, in the case of disc pain, with fluoroscopy.
Shockwave Therapy is another technique offered to patients to deal with pain. It is a newer treatment method and can promote quicker recovery from exercise, injury or surgery. Click here to learn more!
Is regenerative medicine covered by most insurance?
PRP and other forms of regenerative medicine are covered by Workers Compensation and Personal Injury. They are not usually covered by most insurance.
What is the cost of PRP?
The cost of PRP injections can run up to $2,500 out-of-pocket. However, at CSO, we have our own in-office equipment and can offer a very high quality service in a single office visit for $750 per injection.
Unlike many centers offering only regenerative medicine, we offer multi-modal non-operative treatment. Therefore, our practice is not solely dependent upon regenerative medicine as our sole source of income.
Platelet-rich Plasma Therapy
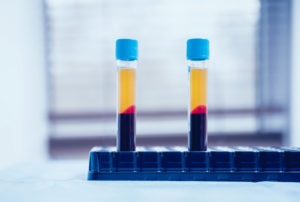
Platelets are kind of like a group of construction workers. When a tear or cut in tissue occurs, the platelets work to create a scaffold, bringing those tissues back together and creating collagen and scar tissue to heal the torn and damaged tissue. Additionally, they release a variety of growth factors and anti-inflammatory cytokines to help induce this healing response and fix the painful problem.
Unlike traditional anti-inflammatory medications, which merely mask the symptoms, PRP offers the opportunity for real healing to occur and problems to be fixed.
What types of conditions are being treated successfully with PRP?
Tendon, ligament and joint injuries are the most common conditions that are being successfully treated with PRP, particularly tennis elbow, plantar fasciitis, knee osteoarthritis (mild or moderate) and rotator cuff tears. Additionally, there is evidence to support PRP’s use in back pain caused by a torn disc. At CSO, we have successfully treated patients with shoulder, neck and back pain with PRP.
“With PRP, my neck pain went from level 8 or 9 down to 2 within three days after my PRP injection.”
—Glenn McKnight, PRP Patient
Is PRP Effective?
Research regarding PRP’s effectiveness shows a wide variety of findings. Factors that influence its effectiveness include:
- A patient’s overall health
- The area of the body being treated
- The quality of the injection
- And placement of the injection at the exact place of injury
At the Center for Spine and Orthopedics, our board-certified specialists with more than 30 years of experience administer PRP very precisely using image guidance with an ultrasound or, in the case of disc pain, with fluoroscopy to ensure that the PRP gets to the exact site of injury.
Typically, only one PRP injection is necessary to be effective. Occasionally, booster shots are required, often depending on whether you re-injure your tissue. It is kind of like fixing a flat tire on your bike. You may be able to fix it and ride another 5,000 miles or you might run over another nail and need another repair.
Generally, it can take up to six or eight weeks to know how effective a single PRP injection has been. The length of time varies depending how quickly an individual heals.
Our specialists recommend PRP as an option when discussing nearly any musculoskeletal pain complaint with their patients, particularly when traditional treatment options have failed or are otherwise not indicated.
CSO Patient Stories
iovera° Pain Treatment
Preventative Relief & Pain Management
The iovera° system creates a “cold zone” that blocks nerve signals and immediately reduces pain without the use of drugs and without permanently damaging nerves.
Many patients can benefit from the long-lasting pain relief of iovera° such as those experiencing pain in the knees, hips, shoulders, ribs, feet and more.
Click here to learn more about this non-surgical pain treatment option and determine if you’d be a good candidate.
Shockwave Therapy
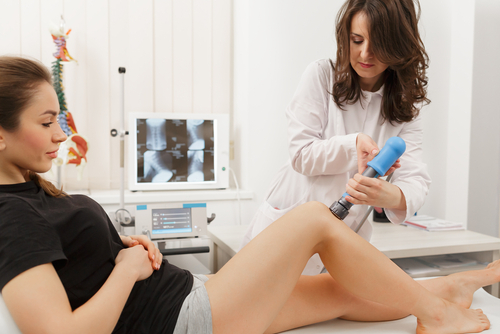
Shockwave is a relatively new treatment for various conditions affecting the muscles and tendons. The pulsating pressure emitted during the therapy works to break up and disperse scar tissue and increase blood flow, which helps to reduce pain and inflammation. Shockwave can also be used to promote quicker recovery from exercise, injury or surgery. It has a very safe track record that leaves no long-term side effects so a patient can benefit from a fast treatment that works both on short term and long-term injury healing.
Programmed Therapy Protocols for the following:
- Tendinitis
- Achilles Tendonitis
- Post muscular injury
- Post ligament injury
- Patellar tendinopathy
- Achillodynia
- Plantar fasciitis
- Heel spurs
- Periostitis / Shin splints
- Post surgical healing
Spinal Injections
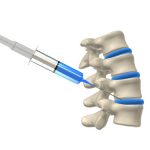
CSO Patient Stories
What are the most common types of injections available?
- Epidural injections
- Facet joint injections
- Sacroiliac joint injections
What are epidural injections used to treat?
Epidural injections are used to treat pain that starts in the spine and radiates to an arm or leg. Arm or leg pain often occur when a nerve is inflamed or compressed (pinched nerve).
Epidural injections involve injecting an anesthetic and an anti-inflammatory medication, such as a steroid (cortisone), near the affected nerve. This reduces inflammation and lessens or resolves the pain. This type of epidural injection is a therapeutic one.
For diagnostic purposes, an epidural spinal injection can be done at a very specific, isolated nerve site to determine if that particular nerve is the pain source. Sometimes only an anesthetic is injected. The immediate response to the injection is closely monitored. If the pain is completely or nearly completely relieved, then that specific nerve is the primary cause of the pain symptoms. If there is little pain relief, then another source of pain exists.
What are facet joint injections used to treat?
Facet joint injections can be done for diagnostic and therapeutic reasons and are often used when pain is caused by degenerative/arthritic conditions or injury. They are generally used to treat neck, middle back or lower back pain. The pain does not have to be exclusively limited to the midline spine as these problems can cause pain to radiate into the shoulders, buttocks or upper legs.
For diagnostic purposes, facet joints can be injected with an anesthetic directly into the joint or by anesthetizing the nerves carrying the pain signals away from the joint (medial branches of the nerve). If the majority of pain is relieved with anesthetic into the joint, then a therapeutic steroid injection may provide lasting neck or low back pain relief.
If anesthetic injections indicate that the nerve is the source of pain, the next step is to block the pain signals more permanently. This is done with radio frequency ablation (damaging the nerves that supply the joint with a “burning” technique).
How are sacroiliac joint injections used?
The SI joints are located between the sacrum and ilium (pelvic) bones. Problems in the SI joints have been shown to cause pain in the low back, buttock and leg. Typically, one joint is painful and causes pain on one side of the lower body. Less often, both SI joints are painful at the same time.
Similar to facet joint injections, the sacroiliac (SI) joint can also be injected for diagnostic and therapeutic purposes. Anesthetizing the SI joint by injection under x-ray guidance is considered the gold standard for diagnosing SI joint pain. A diagnostic injection of the sacroiliac joint with anesthetic should markedly diminish the amount of pain in a specific location of the low back, buttock or upper leg.
A therapeutic injection usually includes a steroid medication with the goal of providing longer pain relief.
When should spinal injections be avoided?
Some people are not good candidates for spinal injections, including people with:
- Skin infection at the site of needle puncture
- Bleeding disorder or anticoagulation
- Uncontrolled high blood pressure or diabetes
- An allergy to contrast, anesthetics or steroids
More information (http://orthoinfo.aaos.org/topic.cfm?topic=A00560)
Diabetic Peripheral Neuropathy
How can Diabetic Peripheral Neuropathy be treated?
Treatments may include pain relievers, anti-seizure medications, topical treatments, and antidepressants. Exercise can also lower blood sugar levels and muscle weakness by slowly building up a person’s muscles to normalcy.
At Center for Spine and Orthopedics, Dr. Leo specializes in advanced treatment in Diabetic Peripheral Neuropathy. For more information on treatment, click here to contact us and schedule an appointment.

Injuries or diseases that affect nerves and muscles can slow or halt the movement of these electrical signals. If you have pain, weakness or numbness in your back, neck or hands, measuring the speed and degree of electrical activity in your muscles and nerves can help your doctor make a proper diagnosis. This process is called electrodiagnostic testing.
What are the most commonly tests used?
Two of the most commonly used tests are:
- Electromyography (EMG) – An EMG records and analyzes the electrical activity in your muscles. It is used to learn more about the functioning of nerves in the arms and legs. When a normal muscle is at rest, it is electrically silent. During an EMG, small, thin needles are placed in the muscle to record the electrical activity. Your doctor will listen and watch a TV-like screen that broadcasts the electrical signals.
- Nerve conduction studies (NCS) are used to find damage to the peripheral nervous system, which includes all the nerves that lead away from the brain and spinal cord and the smaller nerves that branch out from those nerves. This test is often used to help find nerve problems such as carpal tunnel syndrome or Guillain-Barré syndrome.
Radiofrequency Ablation
As with many spinal injections, radio frequency ablation is best performed under fluoroscopy (live x-ray), which our physiatrist uses to guide him in properly targeting and placing the needle. During the procedure, our physiatrist numbs the targeted nerves to minimize pain uses radiofrequency waves to heat the tip of the needle, which he then uses to create a lesion that disrupts the nerve’s ability to send pain signals.
